When your liver can't do its job, your brain starts to pay the price. Hepatic encephalopathy (HE) isn't a disease you can see in a mirror. It doesn't show up on an X-ray. But it can make you forget your own name, confuse day for night, or suddenly act out of character. If you or someone you care about has cirrhosis or advanced liver disease, this is something you need to understand - not just as a medical term, but as a real, daily threat.
What Exactly Is Hepatic Encephalopathy?
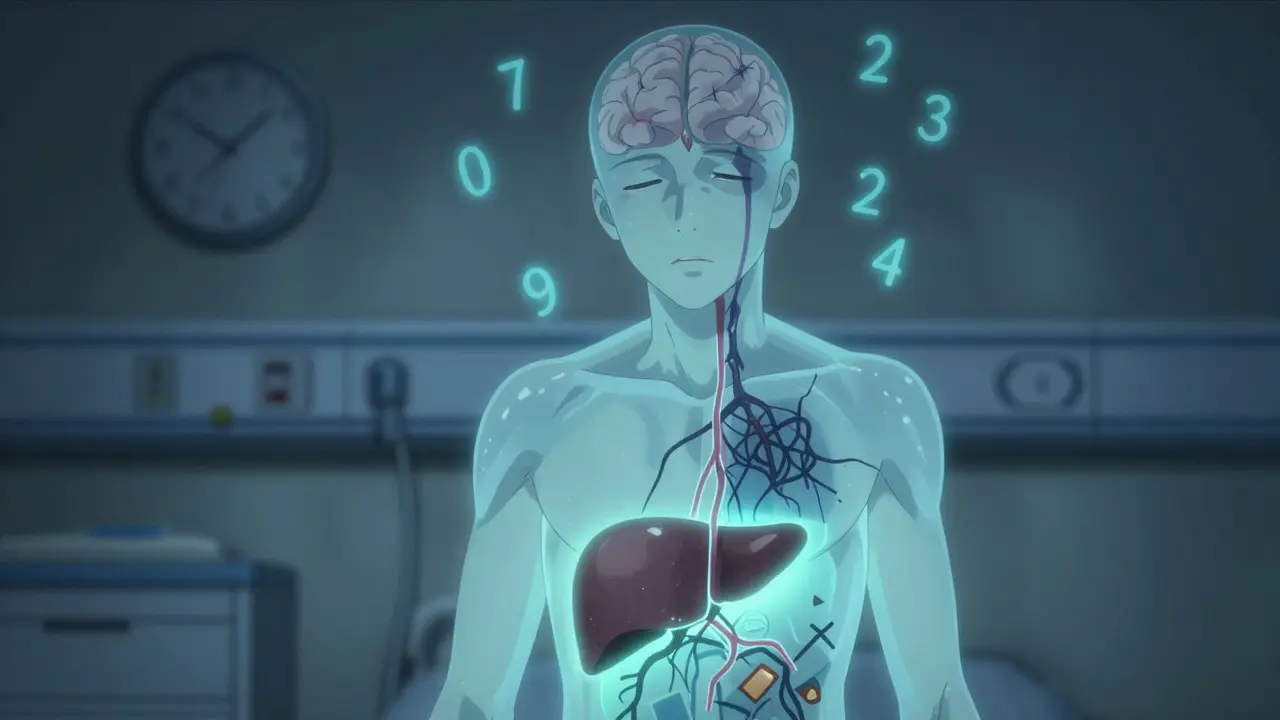
Hepatic encephalopathy is when toxins - mostly ammonia - build up in your blood because your liver can't filter them out. That ammonia travels to your brain, and suddenly, your thinking, mood, and even movement get messed up. It's not dementia. It's not Alzheimer's. It's liver failure showing up in your mind.
Think of your liver like a water filter. When it's healthy, it traps bad stuff before it gets into your bloodstream. But when cirrhosis sets in, that filter breaks. Some blood even finds shortcuts - called portosystemic shunts - that bypass the liver entirely. That means ammonia from your gut goes straight to your brain. And once it's there, it causes swelling in brain cells, messes with neurotransmitters, and scrambles your signals.
There are three types. Type A happens fast - usually after sudden liver failure from an overdose or infection. Type B is rarer: it's when shunts exist without liver damage. But Type C? That's the one most people deal with. It's tied to long-term cirrhosis. About 30% to 45% of people with cirrhosis will have an episode of overt HE. And up to 80% have subtle, silent changes only special tests can catch.
The Warning Signs: From Subtle to Severe
HE doesn’t hit you like a storm. It creeps in. At first, it’s just trouble sleeping. Then you start mixing up words. You forget appointments. You get irritable for no reason. These are Grade 1 symptoms - mild confusion, sleepiness, or trouble concentrating. Most people brush it off as stress or aging.
By Grade 2, things get clearer. You might forget where you are. Your personality shifts - you become withdrawn or overly cheerful. Your speech gets slurred. Family members often notice this before doctors do. A 2021 study found families pick up on changes 48 to 72 hours earlier than clinicians.
Grade 3? You’re confused, incoherent, maybe even drowsy. You can’t follow a conversation. Grade 4 is coma. This is a medical emergency.
And here’s the catch: ammonia levels don’t always match how bad you feel. Some people with high ammonia act fine. Others with normal levels are deeply confused. That’s why doctors don’t rely on blood tests alone. They look at your liver function (bilirubin, INR, albumin), rule out strokes or infections, and watch how you behave.
Why Lactulose Is the First Line of Defense
Lactulose has been the go-to treatment since 1966. It’s not fancy. It’s not expensive. A month’s supply costs $15 to $30. And it works.
Lactulose is a synthetic sugar your body can’t digest. When you swallow it, it travels to your colon. There, good bacteria break it down, producing acids. That drops the pH of your gut from 7 (neutral) to 5 or 6 (acidic). In that acidic environment, ammonia turns into ammonium - a form your body can’t absorb. Instead of entering your blood, it gets flushed out in your stool.
The goal? Two to three soft stools a day. That’s the sweet spot. Too few? Ammonia builds up. Too many? You’re dehydrated and miserable.
Dosing is tricky. Most people start with 30 to 45 mL (about 2 to 3 tablespoons) three or four times a day. But it’s not one-size-fits-all. A 2023 study from the University of Michigan found 65% of people who didn’t respond to lactulose were actually taking too little - under 30 mL per day. That’s not enough to work.
And yes, it’s messy. About 79% of patients say diarrhea is a problem. Nearly two-thirds get cramps. Half hate the taste - it’s sweet, but in a weird, artificial way. One Reddit user wrote: "Lactulose saved me from hospitalization, but the constant bathroom trips ruined my job interviews."
But here’s the thing: if you skip it, you risk ending up in the hospital. Or worse. That’s why sticking with it matters more than you think.

What Happens When Lactulose Isn’t Enough?
For many, lactulose alone isn’t enough. That’s where rifaximin comes in. Approved in 2010, this antibiotic doesn’t get absorbed into your blood. It stays in your gut and kills the bad bacteria that make ammonia - especially Klebsiella and Proteus.
The RIFHE study showed rifaximin cuts recurrent HE episodes by 58% compared to placebo. It’s usually taken as 550 mg twice a day. But it’s expensive - around $1,200 a month. Insurance often covers it, but only if you’ve already tried lactulose and still have flares.
Some patients get better with a combo: lactulose + rifaximin. That’s now the standard for preventing repeat episodes. The European and American liver societies agree on this.
There are other options too. L-ornithine-L-aspartate (LOLA) helps your liver process ammonia by boosting the urea cycle. It’s used more in Europe and Asia. And new treatments are coming. Fecal transplants - yes, poop from a healthy donor - have normalized ammonia in 70% of tough cases. A new oral adsorbent called AST-120, approved in Japan, traps ammonia before it leaves your gut. And a drug called SYN-004, which targets gut bacteria without killing them, showed promise in a 2023 trial.
Prevention Is About More Than Medication
Most people think HE just "happens." But it usually doesn’t. It’s triggered.
Here are the top three culprits:
- Infections - especially spontaneous bacterial peritonitis (SBP). This causes 25-30% of HE episodes. A simple UTI can do it too.
- Bleeding - from the stomach or esophagus. Blood in the gut turns into ammonia. That’s why doctors check for varices.
- Electrolyte problems - low potassium or sodium. Diuretics (water pills) can cause this. Too much salt restriction? Also dangerous.
One caregiver on Reddit tracked her husband’s episodes for months. She noticed every time he got a urinary infection, HE followed. Now she tests him monthly. It’s cut his flares by 80%.
And don’t forget what you eat. You might think you need to cut protein. But that’s outdated. The latest guidelines say: during an acute flare, limit protein to 0.5 grams per kilogram of body weight. But long-term? You need 1.2 to 1.5 grams per kg. That’s about 70 to 100 grams a day for most people. Think eggs, chicken, beans. Protein helps your liver repair itself.
Avoid alcohol. Avoid sedatives. Avoid benzodiazepines. These drugs increase HE risk by over 3 times. If you’re on them for anxiety or sleep, talk to your doctor. There are safer options.

Real-Life Challenges: Adherence, Misdiagnosis, and Isolation
Here’s the ugly truth: 48% of HE patients don’t take their meds correctly. Why? Side effects. Cost. Confusion. The same confusion that caused the problem makes it hard to remember pills.
And many are misdiagnosed. The British Liver Trust found 31% of patients were told they had dementia before anyone checked their liver. That delay can be deadly.
Then there’s isolation. Over 40% of HE patients say they’ve stopped seeing friends because they’re embarrassed by their behavior. One man stopped going to church because he’d suddenly forget prayers mid-service. Another woman didn’t answer calls from her grandchildren because she couldn’t follow the conversation.
That’s why family education matters. Teach them the signs. Show them how to check for confusion - ask simple questions: "What’s your name? Where are we? What day is it?" If they’re wrong on two or more, it’s time to act.
What’s Next? The Future of HE Care
The field is moving fast. In April 2023, the FDA approved a new combo pill: lactulose + rifaximin in one tablet. That’s a game-changer for adherence.
Researchers are also developing blood tests that predict HE risk with 85% accuracy using 12 biomarkers. And smartphone apps like EncephalApp let you test your brain function in 5 minutes - no doctor needed. One trial showed using it cut hospital visits by 62%.
But the biggest shift? We’re no longer just treating ammonia. We’re fixing the gut. The gut-liver-brain axis is now the focus. It’s not just about the liver anymore. It’s about the bacteria inside you.
By 2030, experts predict a 30% drop in HE deaths - not because of new drugs, but because we’re catching it earlier. Not in the ER. Not in the ICU. At home. With a simple test. With a pill you take every day. With family who knows what to look for.
Bottom Line: Don’t Ignore the Signs
Hepatic encephalopathy is preventable. It’s manageable. But it won’t go away on its own. If you have cirrhosis, ask your doctor about lactulose - even if you feel fine. If you’re already on it, make sure you’re taking enough. If you’re still confused, ask about rifaximin. Track your triggers. Keep a log. Talk to your family.
Your brain is still yours. You don’t have to lose it to liver disease.






Comments
lactulose is a nightmare but it saved my dad's life. 2 stools a day is the sweet spot. too much = bathroom jail. too little = brain fog city. i swear by it.
The gut-liver-brain axis is not just a medical concept-it's a philosophical revelation. Our bodies are not isolated systems. The trillions of microbes within us are silent partners in cognition. To treat hepatic encephalopathy as merely a detoxification problem is to misunderstand the depth of human physiology. We are ecosystems, not machines.
America's healthcare system is broken. In India, we use LOLA and traditional Ayurvedic herbs like Bhumiamla and Punarnava to reduce ammonia. No $1200 pills needed. Why are you Americans so dependent on Big Pharma? 🇮🇳
I read this whole thing. Honestly? It's too long. You say lactulose works but then you say 79% of people hate it. So why is it first-line? And why does nobody talk about how many people just quit because it's unbearable? You mention adherence is 52% but don't explain why. This article feels like a drug company brochure. Also, I've been on it for 3 years. It doesn't work for everyone. End of story.
The gut-brain axis isn't just science-it's poetry. Imagine your colon as a cathedral of microbes, each one a silent monk chanting ammonia into oblivion. Lactulose? It's the bell that rings at dawn. Rifaximin? The holy fire that purges the unclean. And yet... we are still so blind. We fix the liver but ignore the whispering gut. This isn't medicine. This is a spiritual awakening disguised as pharmacology. 🙏
Lactulose is a joke. My cousin took it for 6 months and still ended up in the ER. Why are doctors pushing this ancient syrup like it's magic? And why is rifaximin so expensive? This whole system is rigged. Just say no to Big Liver.
This is so important 🙌 I've been managing my mom's HE for 2 years. The biggest game-changer? Tracking triggers. We started a simple log: sleep, diet, UTI, meds. Within 3 weeks, we saw patterns. No more guessing. Also, protein isn't the enemy. I started giving her eggs and Greek yogurt daily. Her brain fog improved by 70%. Don't fear protein. Fear ignorance. 💪
I'm not just a caregiver-I'm a warrior in the war against ammonia. Every time my husband forgets his granddaughter's name, I feel like I'm losing him to a silent, creeping ghost. Lactulose? It's not a treatment-it's a lifeline tethered to a toilet. And don't get me started on the taste-it's like liquid candy made by a demon who hates joy. But here's the truth: if you don't take it, your brain turns to fog. And once it's gone? You can't get it back. I've seen it. I've cried over it. I've held his hand while he stared at the wall and asked, 'Who are you?' So yes. I take it. Three times a day. Even if it ruins my life. Because his life? It's still worth fighting for.