When your nails start looking weird-yellow, thick, crumbly, or lifting off the nail bed-it’s easy to assume it’s just a fungal infection. But what if it’s not? Nail psoriasis and fungal nail infections look alarmingly similar, yet they’re completely different conditions with totally different treatments. Mixing them up isn’t just frustrating-it can make things worse. About 1 in 10 people worldwide deal with one or both of these issues, and nearly 40% of cases get misdiagnosed. That means hundreds of thousands of people are using antifungal creams for psoriasis, or steroid injections for fungus, and nothing changes. Or worse, their nails get worse.
What’s Actually Happening to Your Nails?
Your nails aren’t just dead tissue. They’re connected to living cells under the skin. When something goes wrong with those cells, your nails show it. Fungal infections and psoriasis attack from different directions, but both mess with nail growth and structure.
Fungal nail infection (also called onychomycosis) is caused by fungi-usually Trichophyton rubrum-that sneak in through tiny cuts or damp environments. These fungi feed on keratin, the protein your nails are made of. Over time, they eat away at the nail from the tip or sides, causing thickening, darkening, and a foul smell. The infection spreads slowly, often taking 6 to 12 months to fully develop. It’s more common in older adults, people with sweaty feet, or those who wear closed shoes all day.
Nail psoriasis is an autoimmune condition. Your immune system mistakenly attacks healthy skin cells around the nail, making them grow too fast-every 3 to 4 days instead of every 30. This causes buildup under and around the nail, leading to pitting, separation, and discoloration. Unlike fungus, it’s not contagious. It’s linked to psoriasis elsewhere on the body. About 80% of people with skin psoriasis will develop nail changes at some point, usually 10 to 15 years after their first skin flare.
How to Spot the Difference
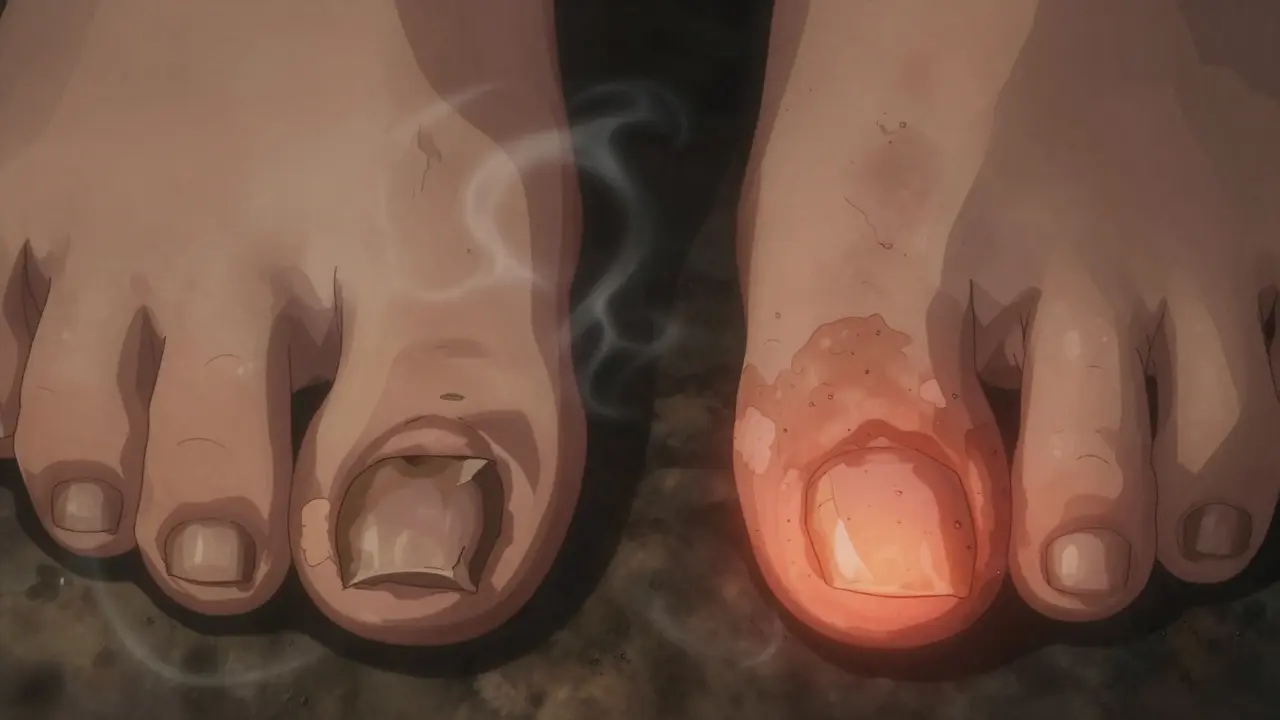
Here’s the truth: you can’t tell just by looking. But there are clues that point strongly in one direction or the other.
- Nail pitting-tiny dents like pinpricks on the surface-is seen in 70% of nail psoriasis cases and only 2% of fungal cases. If you see this, psoriasis is far more likely.
- Foul odor comes from fungal infections in about 40% of cases. Psoriasis never causes this. If your nail smells bad, it’s a red flag for fungus.
- Discoloration can be yellow, brown, or white in both. But psoriasis often shows a salmon-pink patch (called a salmon patch) or oil-drop spots-translucent, oily-looking stains under the nail. Fungal infections usually darken the nail to brown or black.
- Thickening happens in both, but fungal infections cause much more extreme thickening-up to 5mm. Psoriasis thickens nails moderately, around 2-3mm.
- Where it starts matters. Fungal infections typically begin at the tip or side of the nail and creep inward. Psoriasis often hits multiple nails at once, sometimes all fingers or toes, and can appear suddenly without warning.
| Feature | Fungal Nail Infection | Nail Psoriasis |
|---|---|---|
| Primary cause | Fungi (Trichophyton rubrum) | Autoimmune response |
| Most common symptom | Darkening, thickening, foul odor | Pitting, oil-drop spots, nail separation |
| Typical onset | Starts at tip or side, spreads slowly | Affects multiple nails, often sudden |
| Associated with | Footwear, damp environments, age over 60 | Psoriasis on skin or joints |
| Nail thickness | 3-5 mm | 2-3 mm |
| Odor present | Yes (40% of cases) | No |
| Pitting present | 2% | 70% |
Why Misdiagnosis Is So Common
Doctors aren’t always to blame. A 2023 study found primary care physicians correctly diagnose these conditions only 52% of the time. Dermatologists get it right 85% of the time. Why? Because the visual overlap is huge. About 68% of nail psoriasis cases show yellowing that looks exactly like fungus. Patients often come in saying, “I’ve been treating this for months with antifungal cream, and it’s getting worse.” That’s not a coincidence-it’s a red flag for psoriasis.
And it goes both ways. People with fungal infections sometimes get misdiagnosed with psoriasis and prescribed steroid creams or injections. That doesn’t kill the fungus-it can make it worse. One patient on a health forum wrote: “My dermatologist thought it was psoriasis and gave me steroids. My nail got more brittle and started crumbling.”
The problem is compounded by the fact that the two conditions can coexist. About 5% to 30% of people with nail psoriasis develop a secondary fungal infection because the damaged nail bed creates a perfect environment for fungi to grow. This makes diagnosis even trickier.
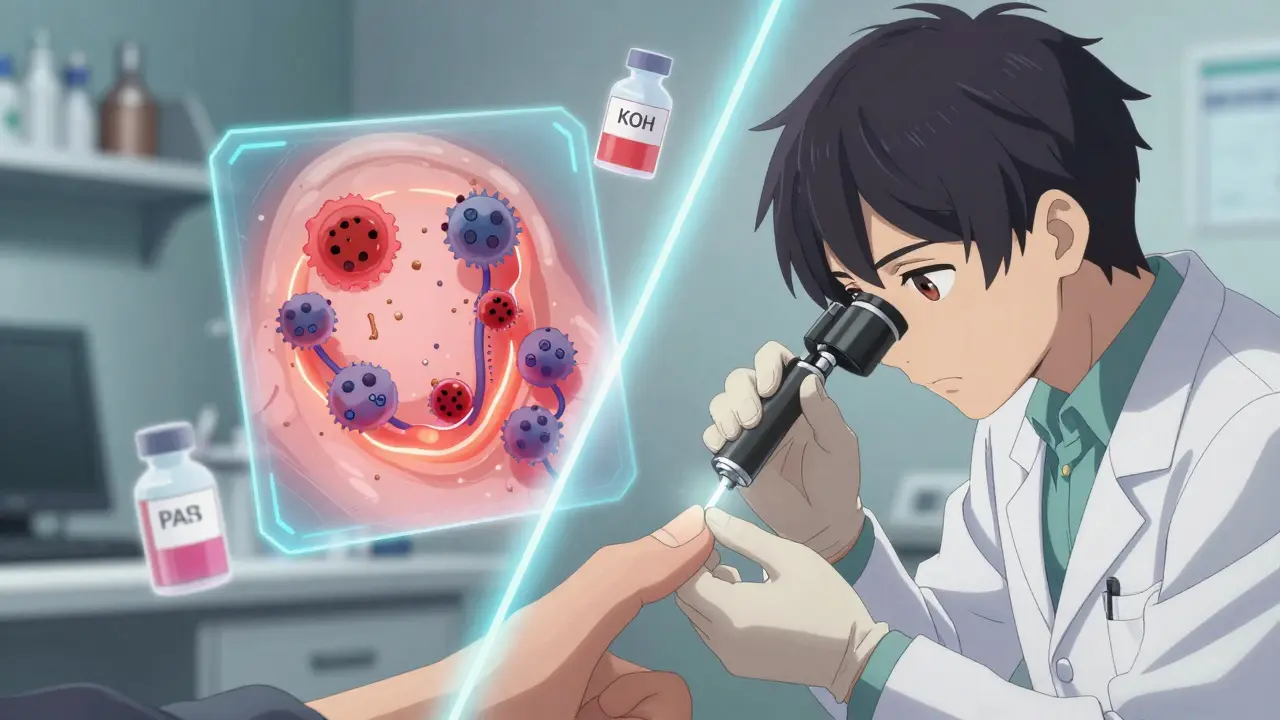
How Doctors Actually Diagnose This
There’s no magic test. Diagnosis requires a combination of visual exam and lab work.
- Clinical exam-The doctor looks for pitting, oil-drop spots, salmon patches, and how many nails are affected. If you have psoriasis on your elbows or scalp, that’s a major clue.
- KOH preparation-A scraping from under the nail is mixed with potassium hydroxide and looked at under a microscope. This test finds fungal elements in 70-80% of cases. It’s fast, cheap, and often the first step.
- Fungal culture-If KOH is negative but suspicion remains, the sample is sent to a lab to grow fungi. This takes 2-6 weeks but is 95% specific-meaning if it’s positive, it’s definitely fungus.
- PAS staining-A special dye highlights fungal cells in nail tissue. It’s 90% sensitive and used when KOH is inconclusive.
- NAPSI score-For suspected psoriasis, dermatologists use the Nail Psoriasis Severity Index. They score four areas of the nail (lunula, matrix, bed, hyponychium) from 0 to 8. A score above 4 usually confirms moderate-to-severe psoriasis.
Advanced tools are emerging. Reflectance confocal microscopy-a non-invasive imaging device-can now differentiate the two with 92% accuracy in early trials. In the future, AI analysis of nail photos and microbiome testing (looking at bacteria and fungi living on the nail) may become routine.
What Works for Treatment
Treatment depends entirely on the diagnosis. Using the wrong one wastes time, money, and worsens symptoms.
For Fungal Nail Infections
- Oral antifungals like terbinafine (Lamisil) are the gold standard. Taken daily for 12 weeks, they clear the infection in 78% of cases, confirmed by culture.
- Topical treatments like efinaconazole (Jublia) or tavaborole (Kerydin) are applied daily for 48 weeks. They work better for mild cases or if you can’t take oral meds.
- Patience is key. Nails grow slowly-about 0.1mm per day. A new, healthy toenail takes 9 to 12 months to grow in completely.
- Home care-Keep feet dry, change socks daily, wear breathable shoes, and avoid walking barefoot in public showers.
For Nail Psoriasis
- Corticosteroid injections into the nail matrix can reduce inflammation. Improvement often shows in 8-12 weeks.
- Topical calcipotriol (a vitamin D analog) applied daily helps reduce thickening and scaling.
- Biologics like secukinumab (Cosentyx) or ixekizumab (Taltz)-drugs that target the immune system-show 65% improvement in nail psoriasis after 24 weeks.
- Emollients like petroleum jelly applied daily prevent the nail from lifting off the bed.
- Avoid trauma-Don’t pick at nails, use nail clippers gently, and avoid manicures that pull on the cuticle.

What Not to Do
Don’t self-treat. Buying antifungal cream off the shelf and slathering it on your nails for months won’t help if you have psoriasis. And don’t assume that because your friend had fungus and it went away with cream, you will too.
Don’t ignore nail changes. Nail psoriasis can be an early sign of psoriatic arthritis. If you have joint pain along with nail changes, see a rheumatologist.
Don’t delay testing. If your nail looks abnormal for more than 3 months, get it checked. The longer you wait, the harder it is to treat.
What You Can Do at Home
- Take monthly photos of your nails under consistent lighting. This helps track changes over time and gives your doctor clear evidence.
- Keep nails trimmed short to reduce pressure and prevent lifting.
- Use a humidifier if you live in a dry climate-dry air worsens psoriasis.
- Wear gloves when washing dishes or using chemicals.
- Track your triggers-Stress, injury, or illness can flare psoriasis. Fungal infections often follow damp exposure.
The Bigger Picture
These conditions aren’t just cosmetic. They affect quality of life. People with nail psoriasis report embarrassment, pain, and difficulty gripping things. Fungal infections can make walking painful. Both can lead to secondary infections if left untreated.
The global market for treating these issues is growing fast-projected to hit $4.1 billion by 2028. But behind those numbers are real people who spent months, even years, on the wrong treatment. A 2023 survey found 78% of psoriasis patients waited over six months for a correct diagnosis. That’s six months of unnecessary creams, frustration, and worsening nails.
There’s hope. New diagnostics are coming. AI tools are being trained to spot the subtle differences in nail images. Microbiome analysis might soon tell us exactly what’s living on your nail-fungal, bacterial, or both.
For now, the best thing you can do is get an accurate diagnosis. If you’ve been struggling with nail changes and nothing’s worked, ask your doctor about testing. Don’t settle for guesswork. Your nails are telling you something. Listen.
Can nail psoriasis turn into a fungal infection?
Yes. Nail psoriasis damages the nail bed and creates gaps where fungi can enter. About 5% to 30% of people with nail psoriasis develop a secondary fungal infection. This is why it’s critical to get the right diagnosis-treating psoriasis with antifungals won’t help, and treating fungus with steroids can make the infection worse.
Is nail psoriasis contagious?
No. Nail psoriasis is an autoimmune condition, not an infection. You can’t catch it from someone else. Fungal nail infections, on the other hand, are contagious and can spread through shared towels, shoes, or public showers.
Why do antifungal treatments fail for some people?
They fail because the problem isn’t fungus. If you have nail psoriasis and use antifungal creams, you’re treating the wrong condition. The underlying immune response continues, and the nail keeps deteriorating. That’s why many patients report their nails getting worse after months of antifungal treatment.
How long does it take to see improvement?
It depends on the condition. For fungal infections, oral terbinafine shows results in 12 weeks, but the nail takes 9-12 months to fully grow out. For nail psoriasis, corticosteroid injections can improve appearance in 8-12 weeks, and biologics like secukinumab show noticeable improvement after 24 weeks.
Can I use over-the-counter treatments for either condition?
OTC antifungals may help very mild fungal cases, but they’re often ineffective for severe infections. They won’t work at all for psoriasis. Prescription treatments are far more reliable. If you’ve tried OTC products for more than 3 months with no improvement, see a dermatologist.
Do I need a blood test to diagnose these?
No. Blood tests aren’t used to diagnose nail psoriasis or fungal infections. Diagnosis is based on physical exam, nail scrapings, and lab tests on nail clippings. Blood tests might be used if psoriatic arthritis is suspected, but not for the nail condition itself.






Write a comment